Secondary glaucoma is the name used to describe glaucomas that occur as a side effect or “secondary” to another underlying medical condition or trauma.
This differs from primary glaucoma, where there’s no identifiable cause for glaucoma to develop.
Even though the causes of primary and secondary glaucomas may be different, the increase in eye pressure and the resulting damage to the optic nerve are the same.
Secondary ocular hypertension (or OHT) is when the eye pressure measurement is higher than the normal range but there is no detectable damage to the optic nerve. Secondary glaucoma is when damage to the optic nerve becomes visible.
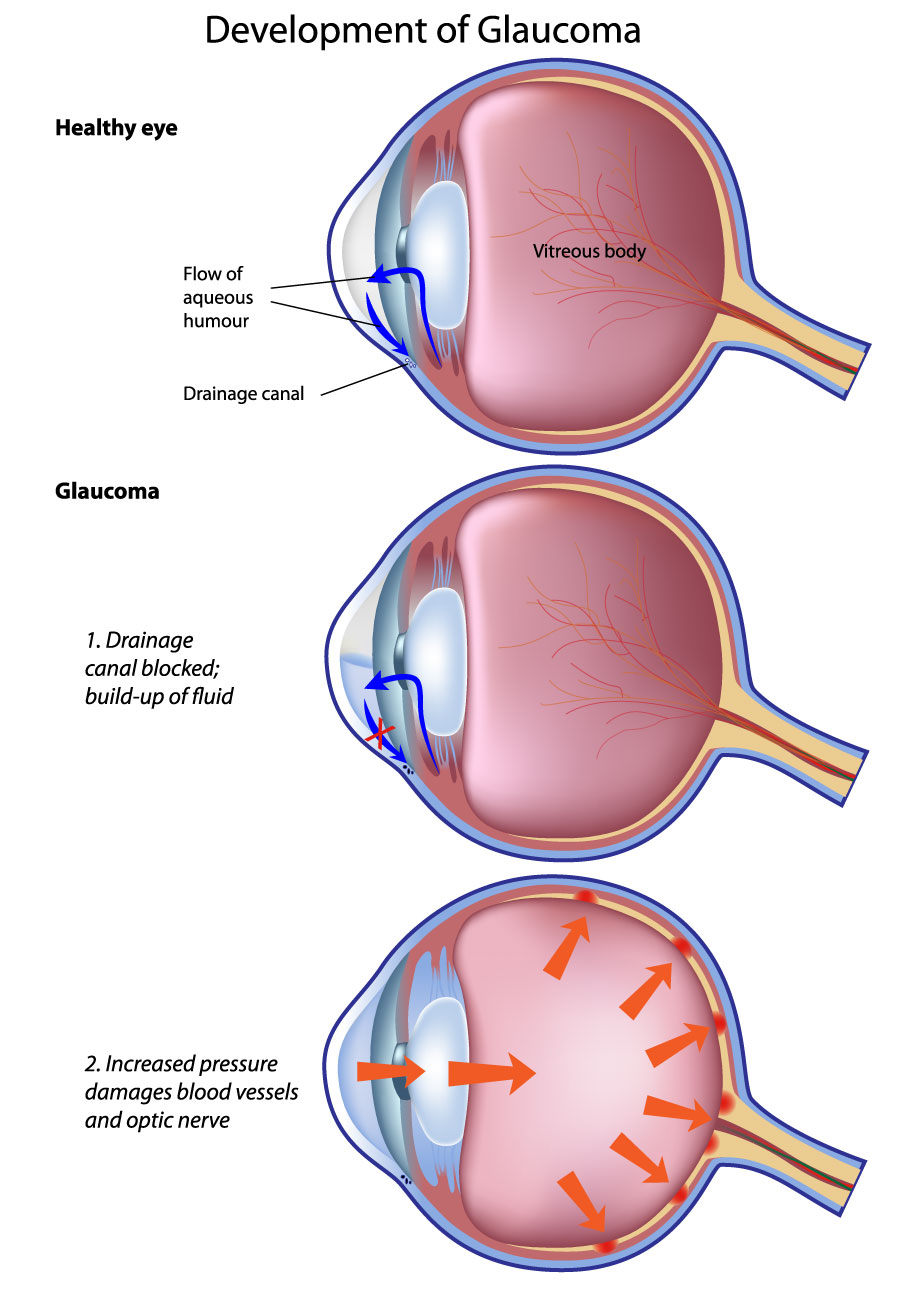
The structure of the eye
To understand secondary glaucoma it’s useful to understand the structure of the eye and how fluid drainage works.
Your eye pressure is controlled by a watery fluid called aqueous humour, or just ‘aqueous’. Aqueous is made in a ring of tissue that sits behind the iris called the ciliary body. It then flows through the pupil and drains away through tiny channels called the trabecular meshwork. The trabecular meshwork is found in the angle between the cornea and the iris (often called the drainage angle). In a normal eye, there is a balance between inflow and outflow of fluid, but in some eyes, this balance is disturbed, and this causes the eye pressure to rise.
In secondary glaucoma, these issues arise due to a problem with the drainage system so fluid outflow doesn’t work as well as it should. The eye can’t get rid of the fluid fast enough and the build-up results in increased eye pressure. The increase in pressure damages the optic nerve by reducing the amount of blood that can get through the tiny blood vessels and by pressing on the nerve itself.
Secondary glaucoma is different to primary open angle glaucoma, in that when the underlying problem that caused the raised pressure is corrected or cured, the pressure may return to normal. If the increased eye pressure has already caused damage to the optic nerve, any resulting sight loss is permanent and irreversible.
Treatment of secondary glaucoma depends on the cause. The aim of any treatment will be to try and bring the pressure down into the normal range to slow down any further damage.
Find out more about treatmentCauses of secondary glaucoma
Pigment dispersion syndrome
Pigment dispersion syndrome occurs when the pigment granules in the iris (the coloured part of your eye) break away and clog up the trabecular meshwork. If the trabecular meshwork is blocked, it is almost impossible for the aqueous to drain effectively and this results in increased eye pressure. This puts extra pressure on the optic nerve and can result in damage to vision. This condition is more common in young, short sighted men.
Pseudoexfoliation
Pseudoexfoliation occurs when the edge of the lens starts to flake away like dandruff, and clog up the trabecular meshwork. The lens sits behind the iris and helps to focus light so we can see clearly. The flaky dandruff stops the aqueous draining away, and this can raise eye pressure and damage the optic nerve. This condition tends to be more common in older people and in people of Scandinavian and Southern Mediterranean origin.
Uveitis
Uveitis occurs when a part of the eye called the uvea becomes swollen and inflamed. If uveitis leads to increased pressure, which then causes damage to the optic nerve, it results in uveitic glaucoma. The uvea is made up of the iris, ciliary body and choroid.
Neovascular
Neovascular (“new blood vessels”) glaucoma occurs when poor blood supply within the eye causes new blood vessels to grow on the surface of the eye and into the drainage channel. The new blood vessels can cause eye pressure to rise by blocking the outflow of aqueous fluid. This type of glaucoma is usually associated with other eye conditions like diabetic retinopathy.
Lens-related issues
Lens-related issues, like cataracts, can also cause a secondary rise in eye pressure. An advanced cataract can swell up and block the flow of aqueous through the pupil and out of the eye. Removing the cataract relives this.
Medicine-related
Medicine-related secondary glaucoma is the result of inflammation caused by medication, typically steroids. Steroids are used for a variety of medical conditions and can be inhaled (inhalers), taken orally as tablets, injected or applied directly to the skin or eye. They are an important type of medicine, but a possible side effect is increased eye pressure. This effect is called ‘steroid response’. This is most common when the steroids are applied locally to the eye, for example when treating uveitis. In most cases of ‘steroid response’, eye pressure will fall back to normal levels when you stop taking the steroids. It is important to have regular eye pressure checks if you are using steroid eye drops for a long time.
Trauma
Trauma can mean either a blow to the eye, a penetrating injury (when something pierces the eye) or a chemical injury (such as an alkali burn). It can happen immediately after the injury or develop over time. Blunt trauma (such as a blow to the eye) can affect the shape of the eye, meaning the pressure builds up over several years. People affected will need to be monitored to limit the chance of developing glaucoma in the future.
Secondary ocular hypertension or increased eye pressure can occur following disease or surgery on the cornea. The cornea is the clear window at the front of the eye. Corneal infections (viral or bacterial) or corneal burns can cause inflammation leading to raised eye pressure.
Other conditions associated with secondary glaucoma include iridocorneal endothelial (ICE syndrome), bleeding inside the eye, raised episcleral venous pressure and tumours.
Iatrogenic
Iatrogenic is when people experience secondary rises in eye pressure following retinal surgery. During retinal surgery, the surgeon may need to put gas or silicone oil in the eye. These substances can have the side effect of raising eye pressure.